REHOVOT, ISRAEL—January 7, 2020—A host of disease-causing viruses called arenaviruses lurk in animal populations in various parts of the world, sometimes crossing over into humans. When they do cross over, they can be lethal, and only very few treatments exist. Researchers led by scientists at the Weizmann Institute of Science have now devised a clever decoy for these viruses that may keep them from spreading in the body.
Two disease-causing arenaviruses – Junín and Machupo – circulate through rodent populations, mainly in South America, and can infect humans when people come in contact with affected rodents. Similar to Ebola, these diseases can cause the body to “bleed out,” and the only treatments to date are risky and complex, as they are taken from the blood of survivors.
The present study, which was reported in Nature Communications, arose from an earlier research question pursued by the group of Dr. Ron Diskin of the Institute’s Department of Structural Biology: how are certain arenaviruses able to move from rodents or other animals into humans? Comparing these viruses with members of the arenavirus family that are not infectious to humans, the researchers noted that the non-infectious viruses did not completely fit a particular receptor – a protein complex on the cell membrane – that serves as an entry point for viruses into human cells. Curiously, however, those that do infect humans were also not a perfect fit. They were just good enough to get by.
This observation led to another insight: perhaps the rodent cell receptors, which were a much better fit to the “entry” proteins on the viruses, could be used to intercept the viruses and lure them away from the human cells. There had been earlier attempts to develop such decoys – “sticky” molecules designed to attract virus proteins – explains Dr. Diskin, but these earlier decoys were based on the structures of human receptors, so they were identical to the ones on the body’s cells and thus unable to compete effectively. In contrast, a molecule based on a rodent receptor, reasoned Dr. Diskin and his team, could far outcompete the human ones for binding to the virus.
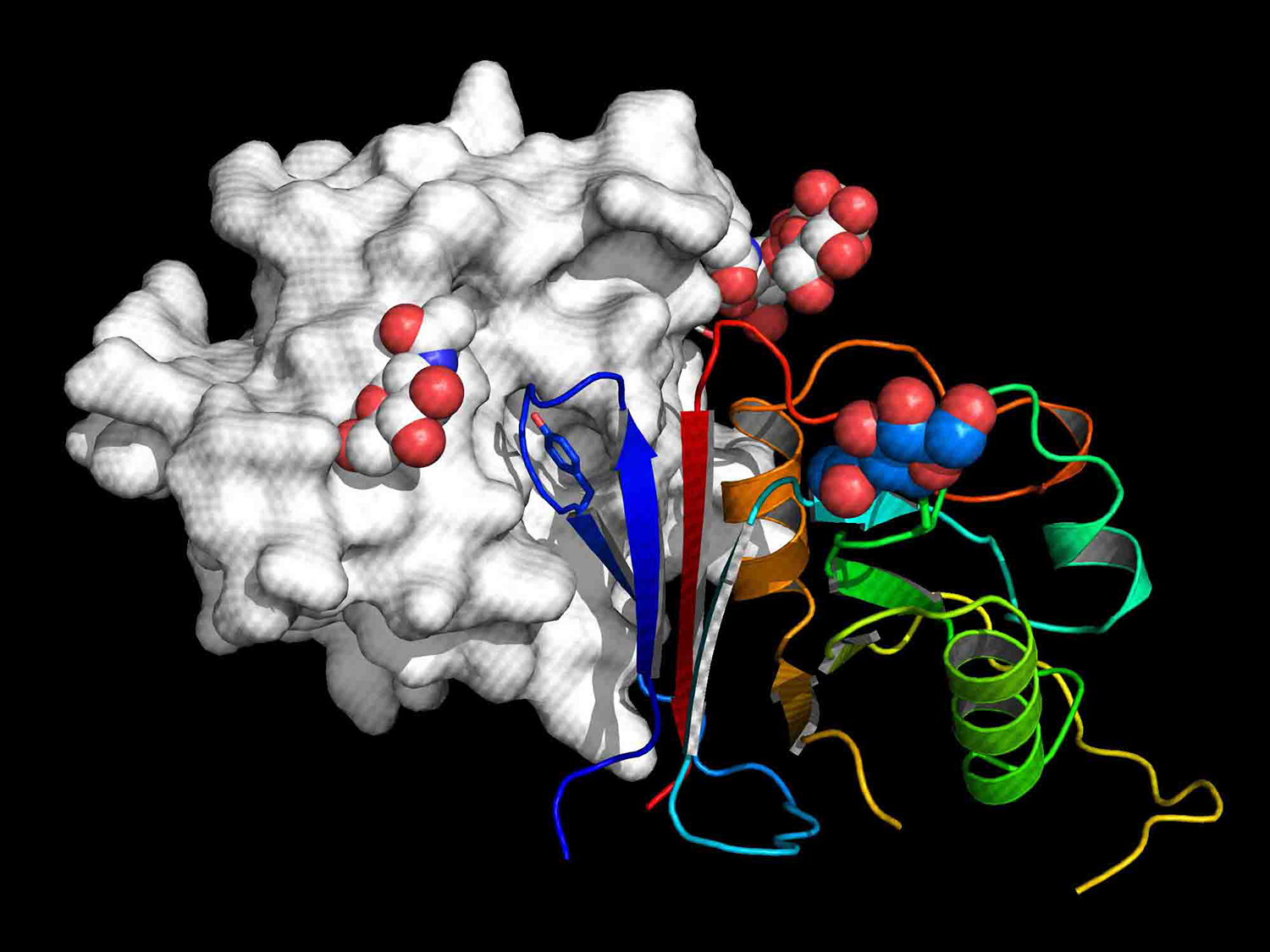
Dr. Hadas Cohen-Dvashi, a member of the Diskin lab, led the next stage of the research, in which she “surgically removed” the very tip of the rodent receptor to which the virus binds and engineered it onto part of an antibody. The newly resulting molecule was called “Arenacept.”

Then the group began testing this molecule – at first against “pseudoviruses,” engineered virus-like complexes that carry the entry proteins but are not dangerous. Even at this stage, the researchers – in collaboration with the group of Dr. Vered Paler-Karavani of Tel Aviv University – noted that Arenacept not only bound strongly to the viruses, it recruited parts of the immune system to mount an attack against the viral invasion.
The next stages of testing took place in labs in the University of Texas, Galveston, and the Institut Pasteur, Lyon, which are equipped to test pathogens at the highest safety levels (BSL-4). Here, Arenacept was pitted against human receptors in lab tests simulating attacks by two of the real pathogenic viruses – the Junín and Machupo viruses.
The researchers found Arenacept to be highly effective at sticking strongly to the viruses before the viruses could bind to the human receptors and, as with the pseudoviruses, they saw the activation of the immune response.
Because Arenacept is based on the entry point shared by all viruses in a given family, rather than on individual characteristics of each virus (as is the case with vaccines or antibodies), it should be equally effective against all the viruses in this family that cross to humans from animals and for viruses that utilize the same receptor. “It might even be effective against viruses from the same family that have not yet been discovered or newly emergent ones,” says Dr. Diskin.
“All signs suggest Arenacept is non-toxic, and that it is also heat-resistant and stable, meaning it could be delivered to the remote areas where these diseases are endemic.” Dr. Diskin reports. “And the idea of creating decoys from mammal receptors might be applied to all sorts of other diseases that cross to humans from animals.” Yeda Research and Development, the Weizmann Institute’s technology transfer arm, has received a patent for Arenacept and is working with Dr. Diskin to advance clinical research.
Also participating in this research were Aliza Borenstein-Katz of the Weizmann Institute of Science; Ron Amon of Tel Aviv University; Krystle N. Agans, Robert W. Cross, and Thomas W. Geisbert of the University of Texas; and Mathieu Mateo and Sylvain Baize of the Institut Pasteur.
Dr. Ron Diskin’s research is supported by the Moross Integrated Cancer Center; the Dr. Barry Sherman Institute for Medicinal Chemistry; the Jeanne and Joseph Nissim Center for Life Sciences Research; and the estate of Emile Mimran.
